

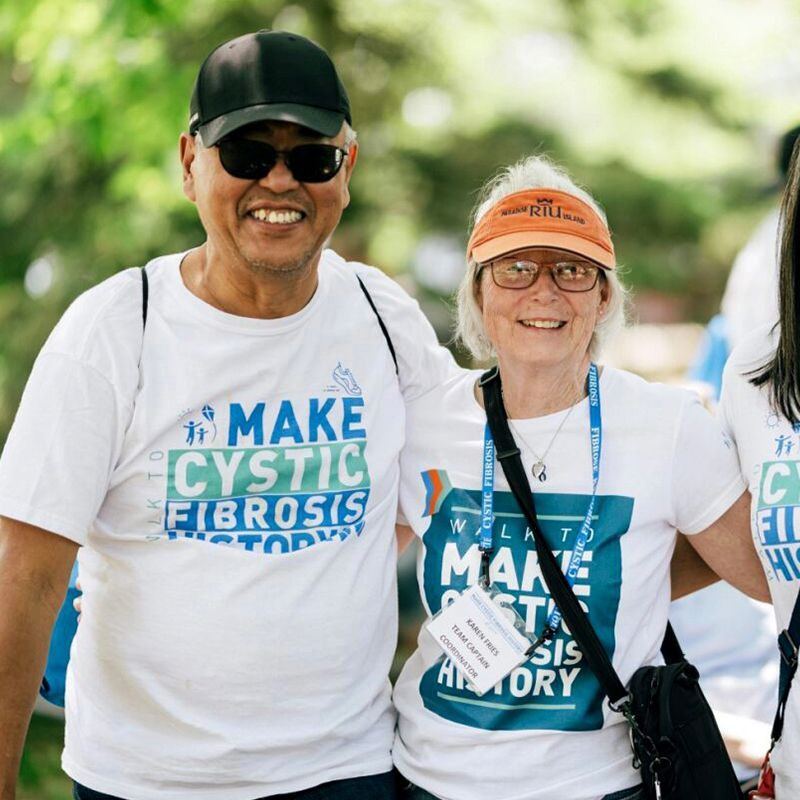

20 Years of Making History
Join thousands of Canadians who are making their steps count on
May 26 by participating in our
20th anniversary
of the Walk To Make Cystic Fibrosis History. Our largest fundraising event takes place in local communities across Canada and brings us together with one goal – taking a
step toward
creating a life unrestricted by CF for ALL Canadians living with cystic fibrosis.

2o Years of Making History
Join thousands of Canadians who are making their steps count on May 26 by participating in our 20th anniversary of the Walk To Make Cystic Fibrosis History. Our largest fundraising event takes place in local communities across Canada and brings us together with one goal – taking a step toward creating a life unrestricted by CF for ALL Canadians living with cystic fibrosis.
And it’s as easy as 1. 2. 3.

1. In Person or Virtual?
Decide if you want to participate virtually or in person on Sunday, May 26

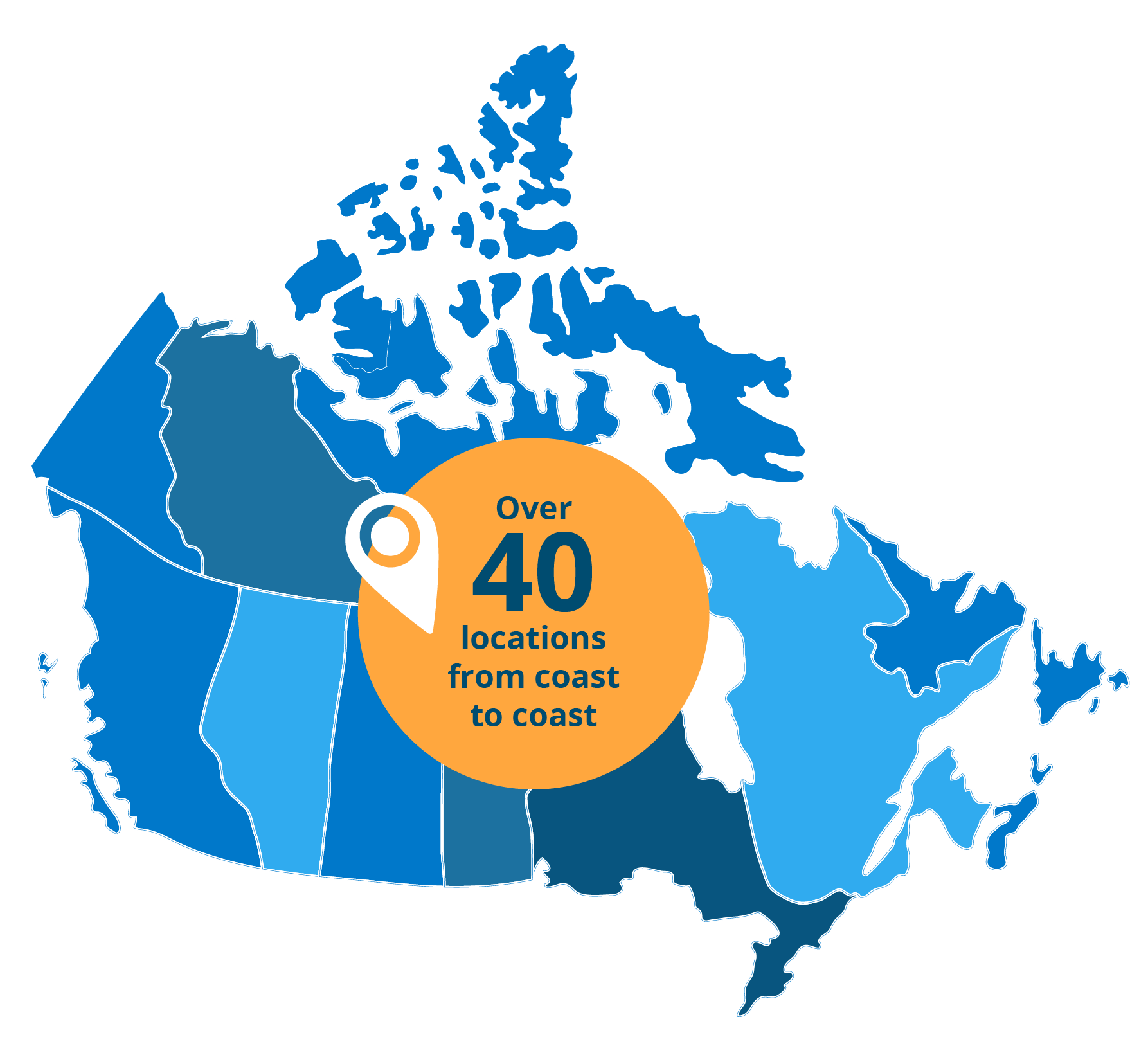
2. Location?
Choose an event location close to home and register.

3. Ready. Set. Go!
Set up your fundraising page and get your (fundraising) party started!

I’ve participated in a few local CF Walks with friends and family as a team bringing awareness for CF. My favourite memories, at the Walk, are seeing the amount of involvement from the community. It was always comforting and brought some hope to the matter.
We keep walking so that every Canadian with CF can live a full, healthy life.
We walk, for people like Chanelle who doesn’t want to be left behind.
Your participation can help to change the cystic fibrosis story in Canada, driving our important work funding CF research, programs and services to lengthen and improve the lives of all Canadians living with cystic fibrosis.
Will you walk with us this year?

The Walk is part of our family's advocacy efforts...
We walk to raise awareness and help find a cure for rare mutations of cystic fibrosis. We want the public to know that there are kids like Sebastian living in Canada who are at risk of being left behind. Trikafta and other modulators are not accessible to all. Sebastian and others who could benefit from these breakthrough medications have the right to try them because the last 5-10% of people living with rare mutations deserve a chance at a longer and healthier life trajectory too.
- Vicky M, Toronto Walk
All kids should have dreams.
My dream is simple. I dream of a future when CF no longer stands for Cystic Fibrosis but rather stands for “Cure Found”.
- Lauren A, Toronto Walk
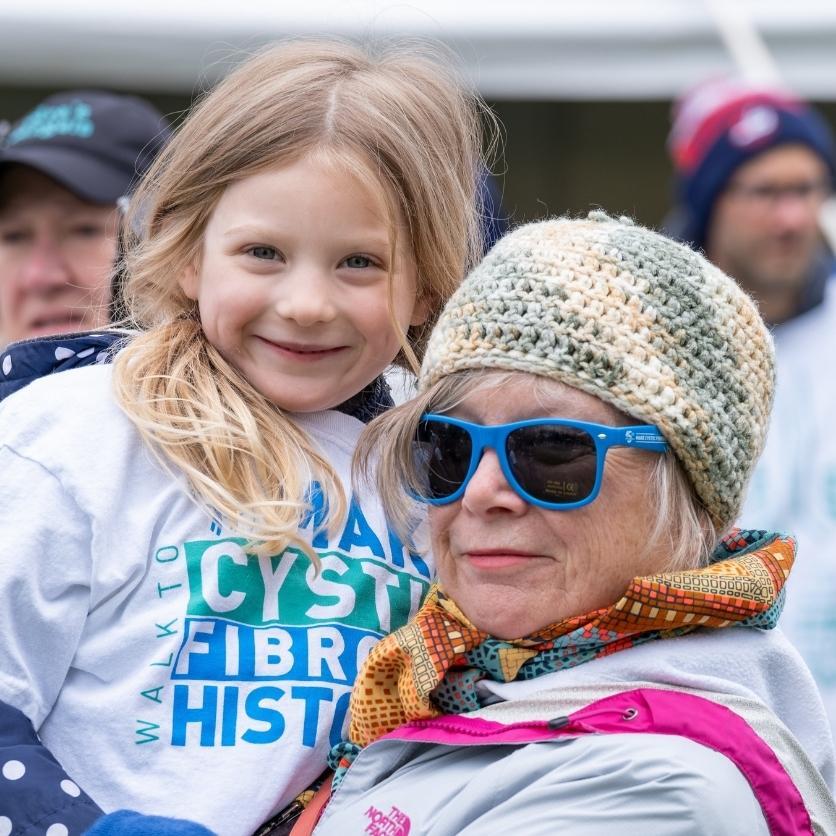

CF Canada works tirelessly...
Thanks to CF Canada and all of their hard work, in 4 short years we have gone from not knowing what the future would hold, to finding hope through gene modulator therapy with the introduction of Trikafta. CF Canada works tirelessly to make medications, like Trikafta, accessible. They support those living with CF and their families. They encourage awareness of the disease. They are also a small organization, and a very small staff team ensures that donations actually help the cause.
> Alissa M, Niagara Walk
© 2024 Cystic Fibrosis Canada. All Rights Reserved
Charitable Registration No. 10684-5100 RR0001



